Overview
Definition
The macula refers to the central portion of the retina or the thin layer of tissue that retains the vision cells in the back of the eye. The retina is similar to film inside a camera. The macula is the central focus point of the retina that allows someone to see fine details such as reading a book.Although age related macular degeneration (AMD) can cause central vision loss, it does not lead to complete blindness. Many patients with age related macular degeneration have no visual symptoms whatsoever and 20/20 vision. A minority of patients will lose central vision and the ability to read and drive a car.
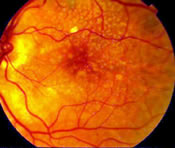 There are two major types of age related macular degeneration. The dry type is the most common form of AMD and affects 90% of patients. The wet type affects only a small percentage of patients, but accounts for the majority of central vision loss due to AMD. Wet AMD implies leakage and bleeding in the macula due to abnormal blood vessels known as choroidal neovascularization (choroidal neovascularization is abnormal blood vessels beneath the macula that leak and bleed and cause central vision loss, blurring of vision, or distortion of vision).
There are two major types of age related macular degeneration. The dry type is the most common form of AMD and affects 90% of patients. The wet type affects only a small percentage of patients, but accounts for the majority of central vision loss due to AMD. Wet AMD implies leakage and bleeding in the macula due to abnormal blood vessels known as choroidal neovascularization (choroidal neovascularization is abnormal blood vessels beneath the macula that leak and bleed and cause central vision loss, blurring of vision, or distortion of vision).
Dry AMD is characterized by drusen, and these are little yellow age deposits that are noted in the macula on clinical examination. Drusen are the hallmark of AMD. Most patients with drusen do not have significant visual changes or vision loss, although it is common for patients to note the need for increased lighting, fluctuating vision, or blurred vision. A minority of patients with dry AMD will advance to central vision loss due to geographic atrophy (geographic atrophy is loss of drusen and other tissues in the macula that are required for good central vision). Unfortunately, there is no cure for geographic atrophy.
There is significant interest in the treatment of wet AMD. New treatments are in evolution for wet AMD to try and reduce leakage and bleeding from choroidal neovascularization. Injection therapies or laser therapies are the mainstays of treatment of wet AMD. In 2006, Lucentis was approved by the US FDA and shown to be the first treatment to improve central vision on average in patients with wet AMD.
Causes and Associations
There are no known proven causes of AMD. It is a degenerative condition that occurs over time and is arbitrarily diagnosed in patients 50 years or older, although drusen can be seen in younger patients. There tends to be familial associations, although just because a family member or blood relative has AMD does not destine someone to have it as well. Over time, the macula accumulates drusen and pigmentary changes, and if choroidal neovascularization or geographic atrophy is avoided, then vision tends to remain good. In a minority of patients, progression to advanced AMD is observed, characterized by geographic atrophy or choroidal neovascularization (wet AMD) and subsequent central vision loss.
Symptoms
Many patients with dry AMD may have no visual symptoms at all. Some patients will require more light to read, have difficulty adjusting between dark and light conditions, notice occasional blurring of vision or fluctuating vision, or notice frank loss of vision. Because AMD affects the macula, the symptoms are typically related to central vision tasks such as reading or driving. Peripheral vision is typically not affected.
Patients with wet AMD may have sudden or slowly or rapidly progressive loss of vision. Leakage and bleeding from choroidal neovascularization typically causes changes in vision, although patients may not be aware of the changes because the other eye may see well. Therefore, it is important to test vision in each eye separately by covering one eye at a time when checking vision.
Some patients with advanced wet AMD may see flickering lights or formed images (an old dog, a familiar face, etc). Flickering lights may be due to chronic leakage in wet AMD. Seeing formed images is not unusual and is a brain response to macular disease.
An Amsler grid (an Amsler grid is a checkered pattern with a central dot in the middle of the pattern) allows a patient to check her vision one eye at a time to monitor for blurring or distortion that may signify wet AMD. Patients with progression of AMD may note changes on the Amsler grid, and if this occurs, they are requested to contact their ophthalmologist promptly.
Examination
Complete and comprehensive ophthalmic examination is important in the assessment of AMD. Patients will receive vision testing, drops to dilate pupils, and a complete examination of the front and back of the eye. Pupillary dilation may create blurring, and therefore, it is often best if a driver accompanies the patient.
What the Doctor Sees
For patients with dry AMD, an ophthalmologist may note drusen accumulation within the macula, pigmentary changes within the macula, or advanced forms of dry AMD such as geographic atrophy. Patients with wet AMD are noted to have fluid in the macula, and hemorrhage or blood is commonly noted as well. There may be larger hemorrhages, and these are typically associated with sudden and severe vision loss. Other blister elevations (retinal pigment epithelial detachments) of fluid in the macula may or may not be symptomatic.
Prognosis
Most patients with AMD will retain good central vision and the ability to read in their lifetime. This is because 90% of AMD patients have dry AMD. This is associated with a more favorable prognosis. Patients with wet AMD may suffer central vision loss. If it affects both eyes with associated vision loss, then the patient may progress to legal blindness, although AMD does not lead to total loss of vision. Thankfully, new treatments are improving the prognosis even for patients with advanced wet AMD.
Prevention and Treatment
Treatment of dry AMD is based on the Age Related Eye Disease Study (AREDS), which demonstrated that a specific formulation of anti-oxidant vitamins and minerals can reduce the risk of progression of dry AMD to more advanced stages and associated vision loss. Daily doses of vitamins in the AREDS study are:
- 500 mg Vitamin C
- 400 IU Vitamin E
- 15 mg Beta-carotene
- 80 mg Zink oxide
- 2 mgxi Copper ode
It is important to check with your medical doctor before starting this AREDS supplement. In general, Vitamin E supplementation should not exceed 400 IU, and smokers should not be on any Beta-carotene supplementation due to an increase risk of lung cancer. There are AREDS formula vitamins available that do not have Beta-carotene that are appropriate for smokers.
Other recommendations noted above include:
- Stop smoking. Smoking has been associated with vision loss and more advanced forms of AMD.
- Eat a diet rich in colorful vegetables and fruits. These food groups have been associated with less advanced AMD and contain anti-oxidants which may slow progression of disease.
- Control blood pressure. High blood pressure is associated with more advanced vision loss and AMD.
- Consider sources of Omega 3 fatty acids. Omega 3 fatty acids found in cold water fish such as tuna and salmon, or those found in fish oil capsules are believed to be associated with less advanced AMD.
- Be physically active. Patients with AMD who were physically active several times a week were at reduced risk for advanced AMD and vision loss.
Prescription and Other Treatment Options
- Lucentis
The prognosis for patients with wet AMD is improving, although there are no cures for AMD. In 2006, Lucentis injection therapy was FDA approved for patients with wet AMD. This is the first treatment shown to improve vision in many patients with wet AMD. Monthly injections are typically performed by a retina specialist and the procedure is relatively painless after eye drop anesthesia. Treatment may need to continue for up to 1 to 2 years depending on the nature of wet AMD. Injections are typically performed in the office setting and carry only a low risk of associated problems such as hemorrhage or infection. Patients who receive injection therapy such as Lucentis will be asked to use topical antibiotics to reduce the risk of infection. Any patient who receives an injection and subsequently has increased pain or loss of vision should contact a doctor immediately. - Avastin
Off-label Avastin injections are also being used to treat wet AMD. Avastin is a drug approved for use in cancer patients. Avastin is designed to shrink blood vessels and therefore shrinks certain cancer tumors after injection of the drug in a peripheral vein. Retina specialists have been performing direct injections of Avastin into the eye, similar to Lucentis and Macugen, to treat wet AMD. There is considerable clinical experience to demonstrate that Avastin may be helpful to patients with wet AMD, but scientific data are less rigorous compared to Lucentis or Macugen therapy. Any injection therapy, even when using only small doses in the eye, can potentially have side effects in the general body. Patients should discuss specific risks and benefits of treatments such as Avastin, Lucentis or Macugen with their eye specialist. - Photodynamic therapy (PDT) with verteporfin (Visudyne)
Photodynamic therapy (PDT) with verteporfin (Visudyne) utilizes an injection of a photosensitizing drug called verteporfin (Visudyne) and a non-thermal laser light to try and reduce leakage from certain types of choroidal neovascularization. It typically does not improve vision as a single treatment, however, it is being explored as an adjunctive agent to Lucentis therapy.PDT is a timed office-based procedure. The Visudyne drug is infused into the vein over 10 minutes and then allowed to collect within choroidal neovascularization over another 5 minutes. The choroidal neovascularization is then exposed to a low energy laser light for about 90 seconds to activate the drug only within abnormal blood vessels in the macula. This produces a chemical reaction within these abnormal blood vessels to reduce blood flow and leakage.
Visudyne clears itself completely from the body over several days. The skin and eyes must be protected from sunlight with clothing and special sunglasses for 2 days after the treatment. No driving is allowed while wearing the sunglasses. Sometimes PDT is combined with other treatments such as Lucentis or with steroid injections to try and attack choroidal neovascularization from several different mechanisms of action.
- Thermal Laser Photocoagulation
Thermal laser photocoagulation may be used in certain cases of choroidal neovascularization where the abnormal blood vessels are not beneath the center of the macula. Thermal laser treatment attempts to heat and destroy choroidal neovascularization but also does affect overlying vision cells. Accordingly, this procedure is typically considered only when the blood vessels are far from the center of the macula. A major problem with thermal laser treatment is recurrent choroidal neovascularization, which can develop in 50-60% of patients. - Low Vision Specialists
Low vision specialists help improve the quality of life for patients whose vision does not enable them to carry out daily activities. For example, AMD patients may have difficulty reading mail or seeing television clearly. Low vision rehabilitation is designed to use specific optical or lighting aids to try and improve specific vision tasks. Although low vision aids are no cure for AMD, they can be helpful in specific vision-related tasks. Low vision specialists can also be a good resource for non-optical aids such as books on tape, large print reading materials, and writing guides.Age Related Macular Degeneration (AMD)
Author: Allen C. Ho, MD
Lucentis therapy works by blocking the growth of choroidal neovascularization and reducing leakage in the macula. Although approximately 70% of patients will maintain or improve vision, and 30% of patients have significant improvement in vision, there can still be vision loss despite Lucentis therapy. Again, Lucentis therapy may involve a series of eye injections, and in clinical trials at 2 years, patients had received 24 injections. Macugen therapy works similarly to slow the growth of choroidal neovascularization and to reduce leakage in the macula. Macugen was the first approved injection therapy for wet AMD.

